2026 Best Humeral Interlocking Nail Options Explained?
In the world of orthopedic surgery, Humeral Interlocking Nails are gaining attention for their innovative design and effectiveness. According to a recent report by the Global Medical Device Alliance, the market for Humeral Interlocking Nails is projected to reach $350 million by 2026. This projection underscores the growing demand for advanced orthopedic tools that promote faster recovery and improved patient outcomes.
Dr. Jonathan Marks, a renowned orthopedic surgeon, emphasized the importance of choosing the right nail for patient-specific needs. He stated, "The success of bone healing often depends on the quality of the Humeral Interlocking Nail used." This highlights the necessity for surgeons to stay informed on the best options available in 2026. As technology progresses, evaluation of these options becomes critical for optimizing treatment strategies.
Yet, not all Humeral Interlocking Nails are created equal. Some designs may lack robustness, leading to complications. Surgeons must reflect on their choices and practices. Understanding the differences between various brands is essential. This guide will explore the top Humeral Interlocking Nail options and their respective benefits and drawbacks, helping to ensure informed decisions in surgical settings.
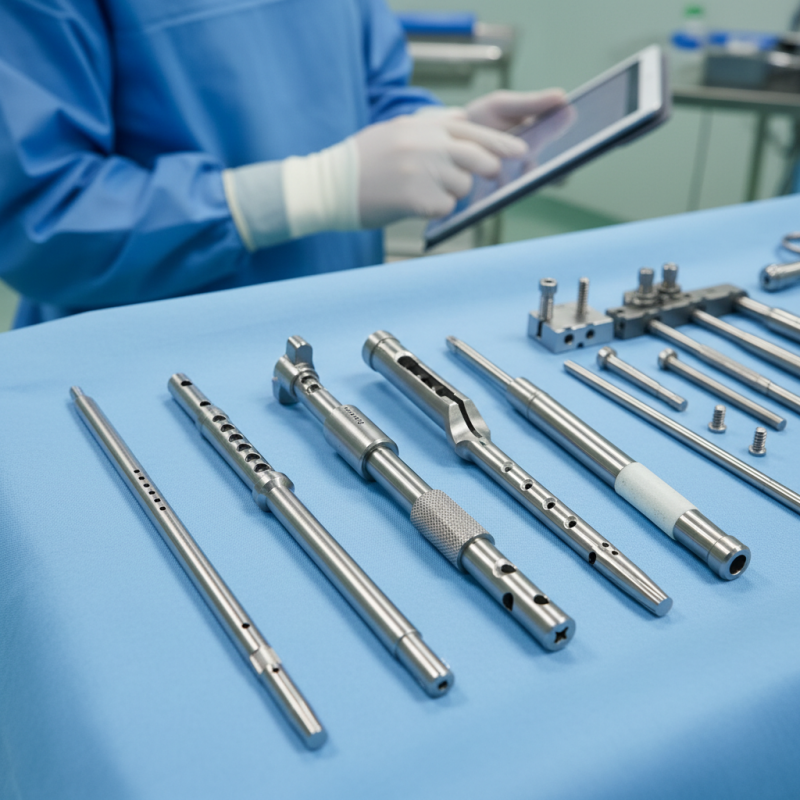
Table of Contents [Hide]
Overview of Humeral Interlocking Nails and Their Uses
Humeral interlocking nails are essential for treating fractures in the humerus. These nails provide stable fixation and help maintain alignment. They are especially useful in complex fractures. Surgeons use them in both intramedullary and extramedullary applications.
The design of these nails allows for varying lengths and diameters. Each option caters to specific patient needs. Surgeons must consider bone quality and potential complications. In some cases, patients might experience discomfort post-surgery. This can lead to a longer recovery period than expected.
Choosing the right humeral interlocking nail is not always straightforward. Factors such as fracture type and patient activity level play a critical role. Monitoring healing progress is crucial. Complications can sometimes arise, so follow-up appointments are necessary. Engaging in conversations with healthcare providers helps clarify concerns.
2026 Best Humeral Interlocking Nail Options
Key Features to Consider When Selecting Humeral Interlocking Nails
When selecting humeral interlocking nails, several key features should guide your decision. First, evaluate the nail's design and material. A stronger nail often improves fixation and promotes healing. Some designs include a locking mechanism, which is vital for stability. This ensures that the nail remains securely in place during the recovery process.
Next, consider the compatibility with existing hardware. An ideal nail should be compatible with various plates and screws. This flexibility can be crucial in complex cases. Additionally, the nail's length and diameter should match the patient's anatomy for optimal fit. A poor fit can lead to complications, making it essential to achieve precise measurements.
Surgeons should also reflect on ease of insertion. A nail that is difficult to position can extend surgery time and affect outcomes. The design should facilitate a smooth insertion process, reducing trauma to surrounding tissues. Consideration of these features can enhance the overall effectiveness of the humeral interlocking nail. Each factor plays a significant role in patient recovery.
Comparative Analysis of Top Humeral Interlocking Nail Options
When considering the best options for humeral interlocking nails, several factors come into play. A comparative analysis reveals key differences in design, material, and functionality. Each option has its pros and cons, influencing surgeon preference and patient outcomes. Some nails offer enhanced stability, while others focus on ease of insertion.
Surgeons often debate the benefits of lightweight materials versus robust designs. Lighter options may reduce the patient's discomfort, but durability is crucial for long-term success. Fitting the nail perfectly with the humeral shaft can be challenging. Small misalignments can lead to complications. Even top choices require careful consideration and skillful hands for proper placement.
Complications after surgery are a real concern. Infection and nonunion can arise with any interlocking nail. Understanding the specific needs and anatomy of each patient is vital. Some techniques work better for certain demographics. This analysis calls for deeper investigation into why some options succeed and others fall short. More studies are needed to refine our approach to these devices.
Surgical Techniques for Implanting Humeral Interlocking Nails
Implanting humeral interlocking nails requires precision and skill. Surgeons must first prepare the surgical site carefully. This often involves making a strategic incision on the lateral side of the humerus. After the incision, exposure of the bone is crucial. This allows for accurate placement of the interlocking nail.
One common technique is the retrograde approach. In this method, the nail is introduced from the elbow, moving upward. It's essential to align the nail with the medullary canal. Misalignment can lead to complications. Surgeons must use fluoroscopy to visualize the nail placement during surgery. This can be complex and sometimes frustrating, especially for less experienced hands.
Postoperative care is another area needing attention. Ensuring the patient follows rehabilitation guidelines can be challenging. Early mobilization is important, but some patients may resist. Close monitoring is vital for detecting potential issues, such as infection or malunion. Reflection on these challenges can enhance future surgical outcomes. Each case is unique, and learning from them is essential.
Postoperative Care and Recovery for Humeral Nail Patients
Postoperative care for patients with humeral interlocking nails is crucial for a successful recovery. Studies show that approximately 70% of complications arise from inadequate postoperative management. Proper care can help mitigate risks. Post-surgery, patients often face issues like pain management, infection, and mobility limitations.
Pain control is essential. Patients should communicate openly about their pain levels. For some, discomfort may linger longer than expected. Regular monitoring can help adjust pain management strategies. It's reported that 60% of patients experience moderate to severe pain in the initial weeks.
Infection prevention is another key aspect. Surgical sites require careful monitoring for signs of infection. Keeping the area clean and dry is vital. Compliance with wound care protocols can reduce infection rates significantly. Mobility exercises, though often painful, are important. They enhance healing and maintain joint function. Yet, some patients may be hesitant to engage in these activities, fearing pain or worsening their condition. Balancing caution with the need for movement is a common dilemma that must be addressed in care plans.